 The temporomandibular joint (also called the jaw joint or TMJ) is one of the most frequently used joints in the human body. These all-too-important joints allow us to speak, chew, yawn, and laugh. So, when our jaws fall victim to injury or dysfunction, it can have devastating effects on our physical, mental, and social health.
The temporomandibular joint (also called the jaw joint or TMJ) is one of the most frequently used joints in the human body. These all-too-important joints allow us to speak, chew, yawn, and laugh. So, when our jaws fall victim to injury or dysfunction, it can have devastating effects on our physical, mental, and social health.
Luckily, calling attention to these overworked (and underappreciated!) joints can help you avoid painful TMJ disorders in the future. And, with November as TMJ Awareness Month, there’s no better time to learn about TMJ health and disorders than now.
In this post, we celebrate and explore all things TMJ. From function to treatment, we’ll tell you everything you need to know about temporomandibular joints.
What is the TMJ?
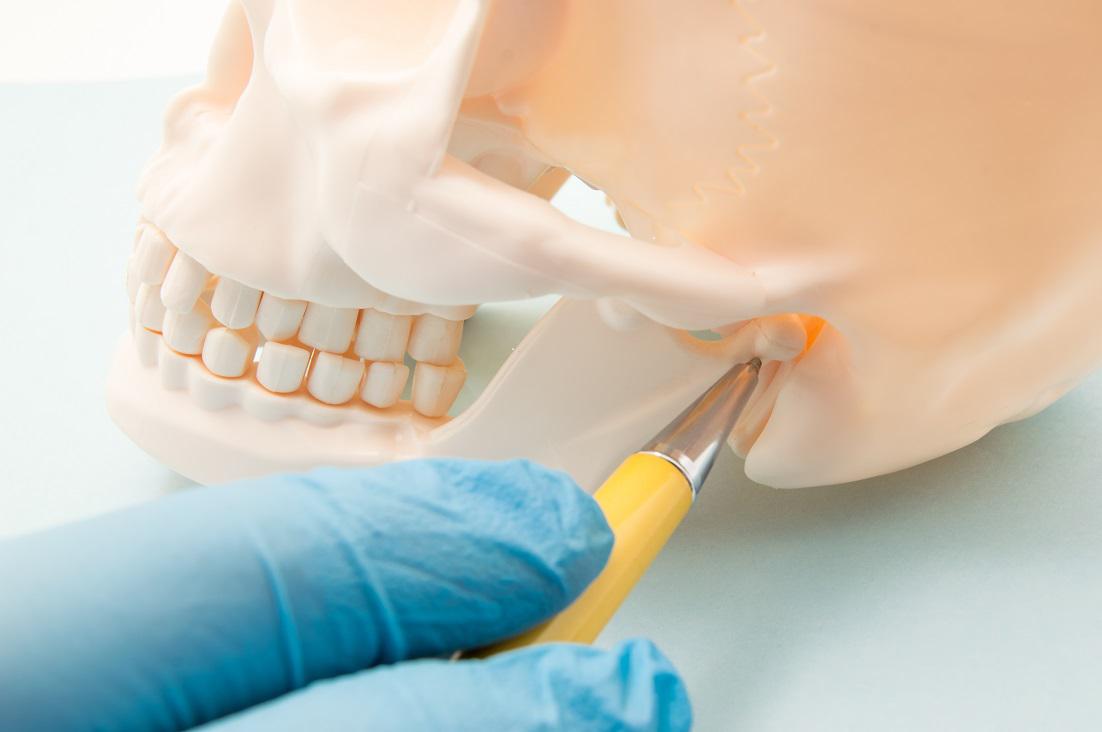
The temporomandibular joint connects the mandible (jaw) to the temporal bone of the skull. The point at which the mandible and skull meet is called the condylar process. The condylar process is the point at which the joint hinges open and closed, which allows us to open and close our mouths.
Medical professionals refer to disease and dysfunction at the condylar process as a temporomandibular joint disorder, or TMD.
What is a TMD?
The temporomandibular joint is incredibly complex. It contains muscles, nerves, bones, and cartilage that all work together in balanced harmony.
But, injury, disease, and disorder in any one of these components can result in a bothersome TMD. Indeed, TMDs can lead to long-term pain and dysfunction that puts your overall health and quality of life at risk.
What are the signs and symptoms of TMJ disorders?
TMJ disorders are relatively common. In fact, experts estimate that nearly a quarter of the population suffers from at least one sign or symptom of a TMD.
Common signs and symptoms of a TMD may include:
- General or localized pain in one or both jaw joints
- Dental pain or sensitivity
- Earaches or tinnitus (ringing in the ears)
- Frequent headaches or migraines
- Pain or difficulty chewing
- Jaw popping, clicking, or locking while eating, talking, or yawning
- Difficulty opening or closing the mouth completely
- Tension or pain in the neck, shoulders, and upper back
- Changes in dental alignment
- Facial swelling or pain
If you are experiencing any of these symptoms, then contact our team. A qualified doctor or dentist can help you diagnose the condition. And, once you have a diagnosis, you can finally learn what is causing the pain and dysfunction.
What causes a TMD?
There are numerous factors that can influence the health of the TMJ, including:
- Sleep bruxism (unconsciously grinding or clenching the teeth while sleeping)
- Dislocation
- Trauma or overuse injuries
- Bite misalignments
- Stress and anxiety
- Arthritis
The cause of a TMD may be the result of one, some, or all of the aforementioned factors. Ultimately, only a skilled medical or dental professional can help you determine the primary cause of a TMD.
How can my healthcare team help me treat a TMJ disorder?
From simple to complex, there are many things your healthcare team can do to treat or manage a TMD, including:
Prescription Medications
Patients with stress-related TMDs may be able to address pain and dysfunction with antidepressants or anti-anxiety medications. In cases of extreme TMJ pain, healthcare providers may recommend prescription-strength painkillers to help patients maintain their quality of life.
Personalized Splints or Night Guards
Splints and night guards are oral appliances that cover the teeth. Both appliances work to protect teeth from damage while also shifting the jaw into better alignment.
The primary difference between splints and night guards is that splints are worn continuously while night guards are worn only at night.
Transcutaneous Electrical Nerve Stimulation (TENS)
Contrary to popular belief, TENS therapy does not deliver painful jolts of electricity. TENS therapy uses weak electrical currents to encourage relaxation in tight jaw muscles. In fact, many patients report only a slight tingling sensation that helps reduce chewing pain by up to 50%.
Radio Wave Therapy
Similar to TENS therapy, radio wave therapy transmits low-level electrical pulses to the face and jaw. These pulses encourage better blood flow, which oxygenates the area and promotes healing.
Orthodontia
Misaligned teeth can place uneven stress on our jaws, which can significantly influence the way the TMJ works. Subsequently, orthodontic treatments (like braces or clear aligners) may be an ideal way for patients to treat occlusion-related TMDs.
Trigger-point and Botox® Injections
Both trigger-point injections (TPI) and Botox injections are clinically proven to decrease TMJ pain and dysfunction.
TPIs deliver pain-reducing medications or sensation-numbing anesthesia to alleviate jaw pain. Botox injections soothe jaw inflammation by reducing the size of the chewing muscle (masseter) and limiting the jaw’s range of motion.
Jaw Surgery
In extreme cases, jaw surgery may be the only way to treat a debilitating TMD. However, healthcare professionals will always start with conservative treatments before recommending surgery.
Prepare for TMJ Awareness Month with a Dental Exam
When it comes to TMDs, prevention is key. So, this year, kick off TMJ Awareness Month with a preventative dental exam with our trusted dentist. Addressing even the subtle signs of a TMJ disorder with a routine exam can preserve your health and quality of life for years to come!